Understanding What Causes Discoloration on Legs
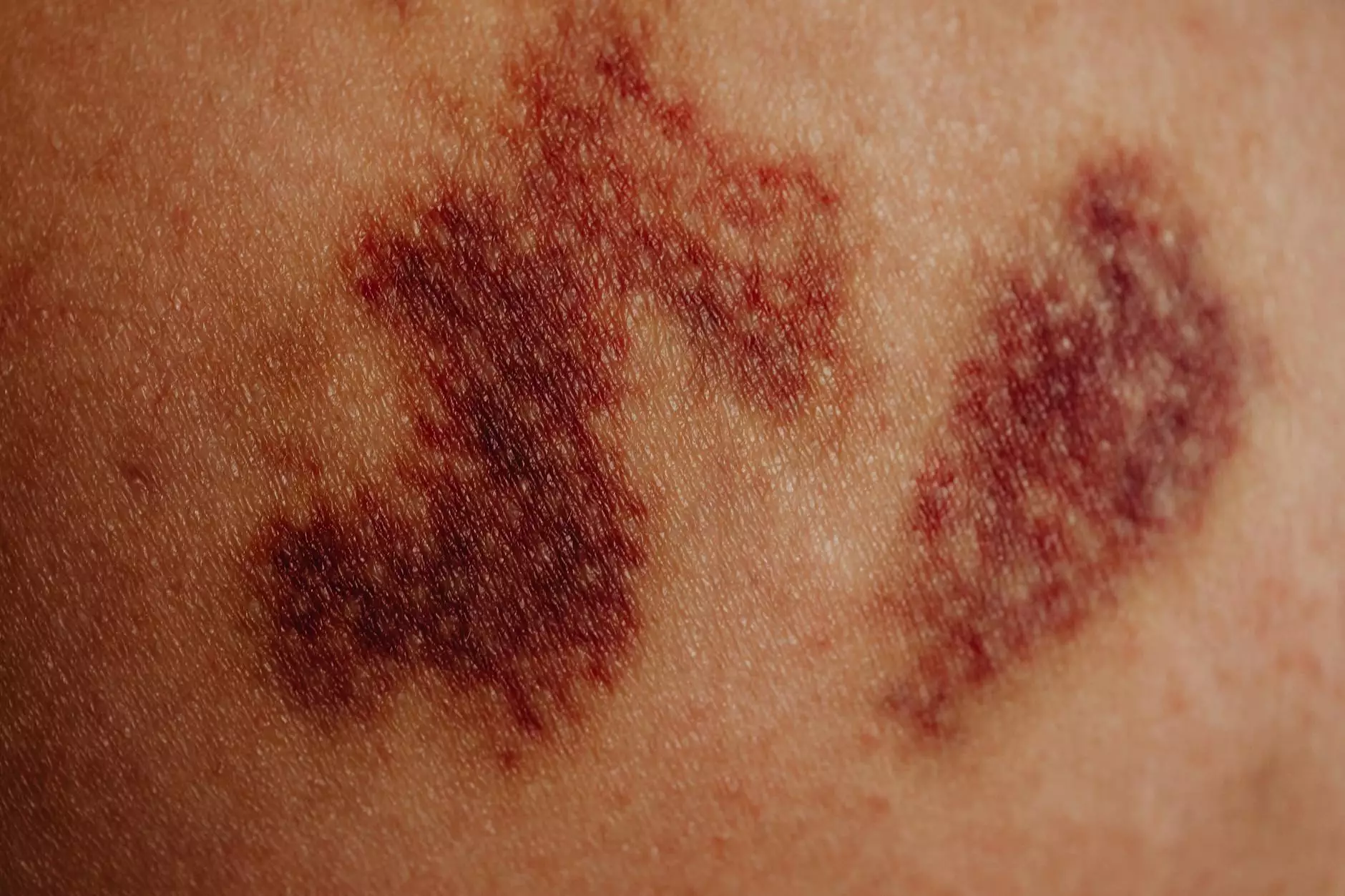
When it comes to our health, our skin often serves as a window into underlying conditions. Discoloration on the legs can be a source of concern, often raising questions about its cause and implications. In this detailed exploration, we will delve into various factors that contribute to discoloration on the legs, enabling you to understand better this common yet complex issue. By the end of this article, you will be equipped with knowledge that not only informs but also empowers you to seek the right medical advice.
What is Leg Discoloration?
Leg discoloration refers to any alteration in the skin color of the legs that deviates from the normal shade. It can present in various formats, including:
- Redness: Indicative of inflammation or vascular issues.
- Browning: Often associated with conditions affecting blood flow.
- Blueness: May signify poor oxygenation in the blood.
- Greyish tint: Could indicate various systemic conditions.
The perception of leg discoloration can vary significantly between individuals, influenced by factors such as skin types, ethnicity, and underlying health conditions. Understanding the causes is essential for proper diagnosis and treatment.
Common Causes of Discoloration on Legs
1. Vascular Issues
One of the most prevalent reasons for discoloration on the legs involves the vascular system. Conditions affecting blood circulation can lead to various skin changes:
- Chronic Venous Insufficiency (CVI): A condition where insufficient blood flow returns to the heart, resulting in pooling and discoloration.
- Varicose Veins: Enlarged veins can cause changes in skin color due to increased pressure and blood pooling.
- Peripheral Artery Disease (PAD): Reduced blood flow can lead to a bluish tint in the extremities.
2. Inflammatory Conditions
Inflammation can also lead to localized discoloration. Various dermatological conditions can cause these changes, including:
- Dermatitis: Skin inflammation that results in redness and discoloration.
- Psoriasis: A chronic inflammatory skin condition characterized by red, flaky patches that can affect limb color.
- Contact Dermatitis: Reactions from contact with irritants can lead to localized inflammation and discoloration.
3. Hyperpigmentation
Hyperpigmentation is when certain areas of the skin become darker in color compared to surrounding skin. This can result from:
- Sun Exposure: UV rays can lead to dark patches known as solar lentigines.
- Post-Inflammatory Hyperpigmentation (PIH): Following an injury or inflammation, the skin may darken as it heals.
- Hormonal Changes: Conditions such as pregnancy can result in increased melanin production.
4. Nutritional Deficiencies
Nutrition plays a crucial role in skin health. Certain deficiencies may cause discoloration, particularly:
- Vitamin B12 Deficiency: Can lead to a pale appearance or patches of darkened skin.
- Vitamin C Deficiency (Scurvy): Can result in discoloration and easy bruising.
- Iron Deficiency Anemia: Can cause paleness and a bluish tint to the skin.
5. Diabetes and Blood Sugar Levels
Diabetes can significantly impact circulation, leading to changes in leg color:
- Diabetic Dermopathy: Characterized by light brown, scaly patches on the surface of the skin.
- Acanthosis Nigricans: Dark velvety patches that can appear in body folds, including the legs.
Identifying Symptoms of Concern
While many forms of discoloration on the legs may be benign, knowledge of alarming symptoms is key to receiving timely care:
- Rapid Color Change: Sudden discoloration could indicate an underlying pathology.
- Accompanied Pain: If discoloration occurs alongside pain, especially sharp or severe pain, medical attention is necessary.
- Ulceration or Skin Breakdown: Open wounds or breakdown may signify serious vascular issues, warranting immediate attention.
When to Seek Medical Advice
It is crucial to approach discoloration with seriousness. Here are situations when you should consult a healthcare provider:
- Persistent discoloration: If the discoloration does not improve or worsens over time, seek help.
- Changes in sensation: Numbness, tingling, or increased sensitivity could indicate nerve involvement.
- Visible lesions or ulcers: Any new growths, bumps, or sores should be evaluated by a doctor.
Diagnosis and Evaluation
Upon visiting a vascular specialist such as those at Truffles Vein Specialists, a thorough evaluation is carried out. This may include:
- Medical History Review: Understanding the patient's history of symptoms, medications, and family health history.
- Physical Examination: Inspection of the legs, noting particular characteristics of the discoloration.
- Diagnostic Imaging: Techniques such as Doppler ultrasound can assess blood flow and vein functionality.
Treatment Options
Treatment for discoloration on the legs will vary based on the underlying cause:
- Compression Therapy: Used for conditions like CVI, it helps improve blood flow.
- Medications: Corticosteroids for inflammation, or topical agents for pigmentation issues.
- Lifestyle Changes: Enhancing diet, increasing physical activity, and quitting smoking can improve overall skin health.
- Surgical Interventions: In cases of severe vein disease, procedures such as sclerotherapy or laser therapy may be considered.
Preventive Measures
Preventing discoloration on the legs involves a multi-faceted approach that includes:
- Regular Exercise: Promotes healthy circulation.
- Wearing Compression Garments: Helps to prevent blood pooling.
- Skin Care: Regular moisturizing and protection from harmful UV rays reduces skin damage.
- Balanced Diet: Ensures adequate nutrition to support skin health.
Conclusion
Understanding what causes discoloration on legs is essential in seeking appropriate treatment and addressing potential health concerns. With a comprehensive approach involving diagnosis, treatment, and preventative measures, individuals can better manage their skin health. If you notice any troubling changes in your legs, do not hesitate to reach out to medical professionals at Truffles Vein Specialists, where experts in vascular medicine can provide the care you need.









